AUTOMATION AGENT
Automate prior authorization status follow-ups with ease
Many healthcare settings, including PT/OT, require follow-ups on prior authorizations initiated by the ordering provider rather than starting a new request. Certain specialties and insurance plans also require the ordering physician to initiate an authorization, leaving the rendering provider responsible for follow-ups. Additionally, there may be times when staff initiates an authorization but lacks the bandwidth to continuously check for updates—leading to delays and administrative strain.
Our Prior Authorization Follow-Up Automation Agent bridges the gap by ensuring seamless tracking of already initiated authorizations.
This specific agent eliminates these inefficiencies by automating high-volume status checks with accuracy through robotic process automation (RPA). This ensures direct updates in your EMR/EHR, reducing administrative burden and improving workflow efficiency.
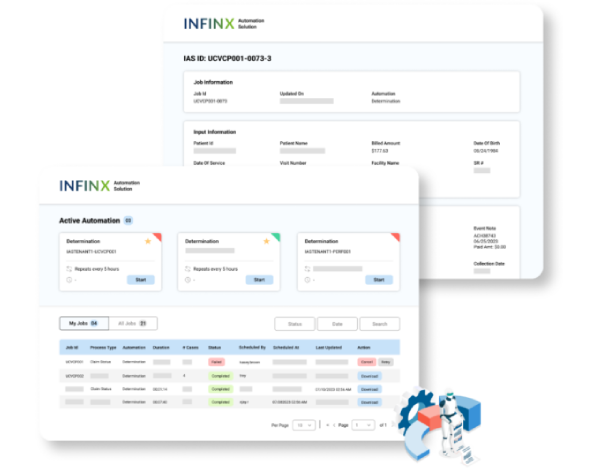
Available as part of our Patient Access Plus platform’s prior authorization module or as a standalone automation agent in our Revenue Cycle Agent Platform, providing the flexibility to automate prior authorization follow-ups in a way that aligns with your existing workflows.
INSTANT AUTHORIZATION UPDATES
Carelon responses delivered directly to your EMR
Automatically track prior authorization requests and receive accurate status updates—without staff intervention.
- Seamless Carelon integration eliminates manual logins and authorization checks by pulling status updates directly into your system.
- Automated EMR updates ensure approved, denied, or pending statuses are reflected automatically, keeping staff informed.
- Scalable automation handles high volumes of authorizations, reducing administrative workload.
With automation agents working 24/7, you can ensure timely and accurate authorization tracking while reducing need for manual follow-ups.
HOW IT WORKS
A fully automated solution for tracking authorization status
Once a prior authorization request is submitted, our automation agent takes over, ensuring timely updates and reducing manual effort.
EMR triggers automation agent
When an authorization request status changes (e.g., Pending Review), the automation agent is automatically assigned the follow-up task.
Authorization status retrieval
The automation agent retrieves the latest status (Approved, Denied, or Pending) directly from Carelon via RPA.
System updated with status
Your EMR/EHR is automatically updated with the latest authorization status, ensuring real-time visibility for your staff.
For denied cases, responses will include a denial letter outlining the reason for the denial, relevant policy criteria, and guidance on the next steps for appeals or resubmission.
Ongoing follow-ups
For unresolved cases, the automation agent re-engages with Carelon at set intervals (e.g., every 6 hours) until a final decision is reached.
With continuous tracking and automated updates, your team can rely on authorization status updates without leaving your system.